The Hidden Truth About Perimenopause Weight Gain (And Why Your “Healthy” Habits Are Failing You)

Sharon Carius
Clinical Nutritionist, Metabolic Balance® Practitioner
4th March, 2026
You wake up at 3:00 AM, heart racing, wondering if the room is actually hot or if it’s just you. You’ve been “being good” – the salads, the morning cardio, the skipped treats – yet the scale is moving in the wrong direction. Specifically, the perimenopause middle has arrived, and it seems entirely uninterested in your willpower.
It’s the great frustration of the 40s: the lifestyle that kept you fit for two decades has suddenly stopped working.
As a clinical expert, I’m here to tell you the truth your GP might have missed: you don’t have a “lack of discipline” problem; you have a biochemical signalling problem. During perimenopause, the decline in estrogen sends your insulin sensitivity into a tailspin. Suddenly, your body is no longer efficient at burning fuel – it’s obsessed with storing it.
This is why generic “menopause diets” fail. They treat the symptom (the weight) without addressing the source (the metabolic shift). To break the cycle of stubborn perimenopause weight gain, we have to stop guessing and start looking at the data.
Whether you are battling perimenopause symptoms like brain fog and fatigue, or you’re ready to finally shed the hormonal weight that won’t budge, the answer lies in your blood chemistry.
Welcome to Advanced Metabolic Health – where we use your unique biology to find the final piece of your weight loss puzzle.
The Hormonal Hijack: Why Your Metabolism Changes After 40
As we cross the threshold of 40, the physiological landscape of the female body undergoes a profound transition. This isn’t merely a byproduct of “getting older”; it is a complex biochemical recalibration. In clinical nutrition, we refer to this as the Hormonal Hijack—a period where the decline of ovarian function begins to disrupt the delicate homeostasis of your metabolic engine.
The Estradiol-Insulin Connection
The primary driver of this shift is the fluctuating, and eventually declining, level of estradiol(E2). Estradiol is not just a reproductive hormone; it is a potent metabolic regulator. Research, including the landmark Study of Women’s Health Across the Nation (SWAN), has demonstrated that the transition through perimenopause is directly associated with an increase in visceral adiposity (fat stored around the midsection) and a decrease in lean muscle mass, independent of age or physical activity.
Clinically, we see a reduction in insulin sensitivity during this window. Estradiol plays a critical role in the translocation of GLUT4—the primary glucose transporter in your muscles. As estradiol levels drop, your cells become less efficient at “opening the door” for glucose. The result? Your pancreas must pump out higher levels of insulin to compensate. Because insulin is your primary fat-storage hormone, these chronically elevated levels act as a biochemical “lock” on your adipose tissue, particularly in the abdominal region.
The Sarcopenia Slide and BMR
Simultaneously, the 40s often mark the acceleration of sarcopenia—the age-related loss of skeletal muscle tissue. Muscle is your most metabolically active tissue; it is the “furnace” where calories are burned. Studies published in the Journal of Clinical Endocrinology & Metabolism indicate that the loss of estrogen and progesterone accelerates the decline of protein synthesis.
When you lose muscle, your Basal Metabolic Rate (BMR)—the number of calories your body burns at rest—drops significantly. This explains why the same caloric intake that maintained your weight at 35 suddenly leads to a 1lb-per-month gain at 45. Your “metabolic floor” has lowered, and your biology is now optimized for energy storage rather than expenditure.
The Adrenal Shift and the Cortisol Trap
Finally, we must address the HPA (Hypothalamic-Pituitary-Adrenal) Axis. As ovarian production of progesterone declines, the body increasingly relies on the adrenal glands to produce hormonal precursors. This puts an immense burden on the adrenals.
If you are lead a high-stress lifestyle, your body remains in a state of chronic hypercortisolemia (elevated cortisol). Cortisol is catabolic to muscle but anabolic to fat. It triggers gluconeogenesis—literally breaking down your hard-earned muscle to create blood sugar, which, thanks to your declining insulin sensitivity, is then promptly stored as belly fat.
The Bottom Line: You aren’t failing your diet; your biochemistry is currently “hijacked” by a hormonal environment that prioritizes survival and storage over vitality and leanness. To reverse this, we cannot simply “eat less.” We must use clinical nutrition to restore insulin sensitivity and signal to your brain that the “crisis” is over.
Estrogen, Insulin, and the “Perimenopause Middle”
The accumulation of weight around the abdomen—often referred to as the “perimenopause middle”—is not a coincidence; it is a direct consequence of the shifting relationship between estradiol and insulin. As ovarian function declines, the loss of estradiol disrupts your body’s ability to manage glucose effectively.
In a healthy metabolic state, estradiol acts as a gatekeeper for insulin sensitivity. It assists in the translocation of GLUT4, the primary transporter responsible for moving sugar out of your bloodstream and into your muscles for fuel. However, as estradiol levels fluctuate and drop during the transition, this “gate” becomes heavy and resistant.
The Shift to Visceral Storage
When your cells become resistant to insulin’s signals, your pancreas overcompensates by pumping out even more insulin to force blood sugar levels down. Because insulin is a powerful anabolic (storage) hormone, these chronically high levels signal your body to protect and expand its energy reserves.
The Study of Women’s Health Across the Nation (SWAN) confirms that this hormonal shift specifically favors the deposition of visceral adiposity—fat stored deep within the abdominal cavity and around vital organs—rather than the subcutaneous fat found on the hips or thighs. This shift happens regardless of your previous body shape or activity level, creating a “metabolic lock” that makes traditional dieting feel like an uphill battle.
Why “Normal” Glucose Isn’t Enough
Many women are told their fasting glucose is “normal” by their GP, yet they continue to gain weight. This is because glucose is often the last marker to break. By looking at Fasting Insulin and the Estradiol-Insulin ratio, we can identify the “Hormonal Hijack” years before it manifests as a clinical issue, allowing us to implement a targeted Advanced Metabolic Health strategy to unlock the middle.
Why “Eat Less, Move More” Is a Recipe for Metabolic Stalls
If you are in perimenopause, the traditional advice to “eat less and exercise more” isn’t just outdated—it’s biologically counterproductive. When you slash calories and ramp up high-intensity cardio, your body doesn’t see a “fitness goal”; it sees a survival threat.
In your 40s, your stress resilience changes. Dropping calories too low triggers the “Starvation Response,” where your thyroid slows down to preserve energy. Simultaneously, excessive exercise spikes cortisol, which signals your body to protect its most valuable energy reserve: belly fat.
Clinically, we see this lead to:
- Metabolic Adaptation: Your body learns to run on fewer calories, making future weight loss nearly impossible.
- Muscle Wasting: Without adequate fuel, your body breaks down muscle for energy, lowering your metabolic rate.
- Hormonal Burnout: You end up “tired and wired”—exhausted but unable to sleep, while the scale remains frozen.
To break a perimenopause plateau, we have to stop the “stress-and-starve” cycle. We don’t need more depletion; we need Biochemical Alignment.
Estrogen, Insulin, and the “Perimenopause Middle”
While the perimenopause middle is often what brings women into my clinic, it is rarely the only symptom they are battling. Perimenopause is a systemic shift; when your sex hormones begin their erratic decline, they take your energy, your mood, and your cognitive clarity with them.
If you feel like a “stranger in your own skin,” it’s not in your head—it’s in your biochemistry.
Brain Fog, Fatigue, and the 3 AM Wake-Up Call
The most common complaints I hear from high-performing women in their 40s are: “I can’t think,” and “I can’t sleep.” This isn’t just “stress”—it’s a disruption of your neuro-metabolic health.
- The Progesterone Drop: Progesterone is your body’s natural “Valium.” As levels plummet, your brain loses its primary calming signal, leading to the 3 AM wake-up call—that sudden, heart-racing alertness that makes a full night’s rest feel impossible.
- Nocturnal Hypoglycemia: Erratic estrogen levels can lead to blood sugar crashes in the middle of the night. Your brain perceives this as an emergency and spikes cortisol to raise your glucose, effectively “bolting” you awake.
- The Cognitive “Static”: Estrogen is highly neuroprotective. Its decline affects the way your brain uses glucose for fuel, leading to brain fog and a loss of executive function that no amount of caffeine can fix.
The Domino Effect: How Hormonal Shifts Trigger Systemic Inflammation
In the clinical world, we know that estrogen is a powerful anti-inflammatory. When its levels become unpredictable, your body loses its primary defense against “metabolic static.”
This triggers a domino effect of systemic inflammation:
- Joint & Muscle Aches: Many women mistake perimenopause for “just getting old,” when in reality, the loss of estrogen increases inflammatory markers like CRP (C-Reactive Protein), leading to unexplained stiffness and pain.
- Digestive Disturbance: Fluctuating hormones alter your gut microbiome and slow down motility. This creates the “perimenopause bloat”—where you feel heavy and inflamed regardless of how “clean” your diet is.
- The Fat-Inflammation Loop: Visceral fat (belly fat) is biologically active; it produces its own inflammatory cytokines. This creates a vicious cycle: Hormonal shifts lead to belly fat, and belly fat leads to more inflammation.
The Clinical Insight: We cannot “exercise away” inflammation. We have to use Advanced Metabolic Health strategies to calm the system, stabilize the blood sugar, and provide the specific micronutrients your body needs to dampen this inflammatory response.
The Clinical Connection: Is Your GP Saying Your Labs are “Normal”?
It is the most common frustration I hear in my clinic: a woman in her 40s feels exhausted, inflamed, and is gaining weight despite no change in her lifestyle, yet her doctor insists her bloodwork is “perfectly normal.”
If you’ve been told there’s “nothing wrong” while your body feels like it’s breaking down, you aren’t imagining things. The problem isn’t your intuition; it’s the standard of measurement.
Standard laboratory ranges are designed to identify disease, not to optimise vitality.
The Gap Between “Standard” Results and “Functional Optimal”
Most medical laboratories determine “normal” ranges based on a statistical average of the population—a population that is, unfortunately, increasingly metabolic-unhealthy. Being “within range” simply means you aren’t in a state of acute medical crisis.
In the Advanced Metabolic Health framework, we look for Functional Optimal Ranges.
This is the narrow window where your biochemistry actually thrives.
- Standard “Normal”: You are not clinically sick (yet).
- Functional “Optimal”: Your hormones are balanced, your cells are sensitive to insulin, and your body is effectively burning fat for fuel.
The gap between these two is where perimenopause symptoms—like the “middle” weight gain and brain fog—live. By catching these “sub-clinical” shifts early, we can reverse the trajectory before it becomes a chronic metabolic condition.
3 Key Metabolic Markers Every Woman Should Test in Her 40s
To bridge this gap, we move beyond basic cholesterol and glucose tests. If you want to solve the mystery of perimenopausal weight gain, these three markers are non-negotiable:
1. Fasting Insulin (The “Fat-Storage” Switch)
Standard labs often only check fasting glucose, which can remain “normal” for years while your body is struggling behind the scenes. Measuring Fasting Insulin (and calculating your HOMA-IR score) reveals how hard your pancreas is working. If this number is creeping up, your body is in “storage mode,” making weight loss biologically impossible regardless of your calorie intake.
2. Hemoglobin A1c (HbA1c)
While glucose is a snapshot of one moment, HbA1c provides a 3-month average of your blood sugar levels. In perimenopause, even slight elevations within the “normal” range indicate glycation—a process that accelerates aging and triggers systemic inflammation. We aim for a functional optimal level (typically below 5.2%) to ensure your metabolism remains flexible.
3. hs-CRP (The Inflammation Gauge)
High-sensitivity C-Reactive Protein (hs-CRP) is a marker of “silent” systemic inflammation. In your 40s, inflammation acts like “metabolic static,” blocking hormonal signals and causing the scale to stick. If your hs-CRP is elevated, your body is too busy fighting internal “fires” to focus on burning fat.
The WNutrition Difference: We don’t just look at these markers in isolation. We analyze how they interact within our 36-marker panel to create your Personalized Nutritional Blueprint, turning “normal” results into an actionable plan for mastery.
How to Stop the Upward Trend and Reclaim Your Energy
Reversing the “perimenopause middle” requires a strategic shift in how—and when—you eat. We focus on signaling to your brain that you are in a state of abundance and safety, which allows your body to finally release its grip on stored fat.
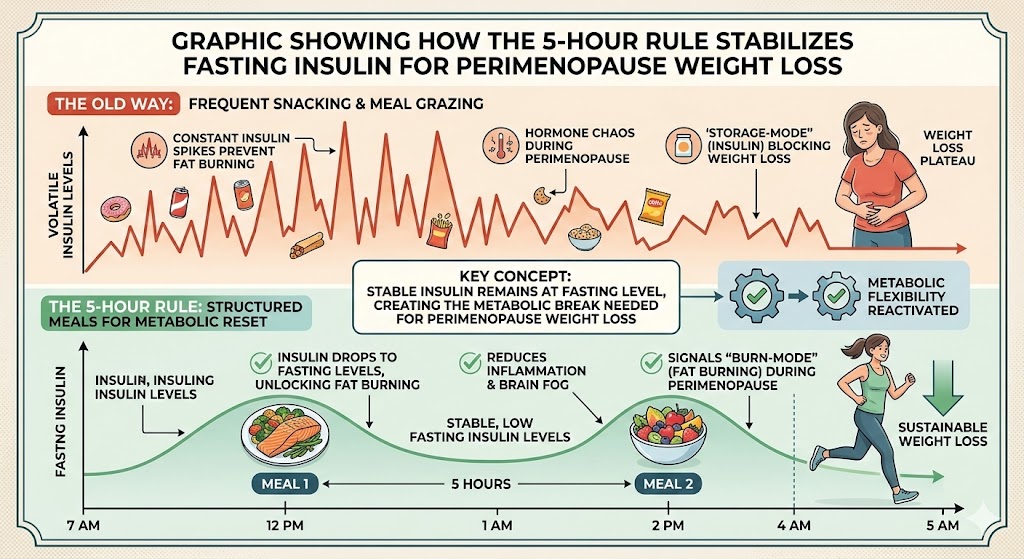
The 5-Hour Rule: Stabilizing Insulin to Unlock Stored Fat
One of the most powerful tools in our clinical toolkit is the 5-Hour Rule. In a world of constant grazing, your insulin levels never have a chance to drop. If insulin is high, fat burning is biologically “locked.”
By allowing exactly five hours between meals, we create a Metabolic Pause. This allows your insulin to return to a baseline level, signaling your body to transition from “Storage Mode” to “Burn Mode.”
- No Snacking: This prevents “Insulin Creep,” where constant small spikes keep you in a fat-storage state all day.
- Deep Cellular Repair: These windows of rest allow your digestive system to reset and your cells to regain their sensitivity to hormonal signals.
Shifting from Deprivation to Nourishment: The 12-Week Reset
The 12-week Advanced Metabolic Health journey is not a “fast.” It is a clinical reset designed to flood your body with the nutrients it has been starved of during years of “Eat Less, Move More.”
- Phase 1 & 2 (The Reset): We eliminate inflammatory triggers and use your blueprint to stabilize blood sugar and reboot your energy.
- Phase 3 (The Flow): We reintroduce lifestyle flexibility, teaching your body how to maintain its new “Metabolic Floor.”
- Phase 4 (The Mastery): You walk away with a permanent understanding of how to fuel your body through the remainder of the menopausal transition and beyond.
We move you from deprivation (which spikes cortisol) to nourishment (which lowers it). When your body feels safe and fueled, the weight doesn’t just “come off”—it stays off.
Frequently Asked Questions About Perimenopausal Metabolism
Navigating the transition of your 40s often brings up more questions than answers. Here are the most common clinical concerns I address with my clients regarding their metabolic health.
Can I actually lose weight in perimenopause without HRT?
Yes. While Hormone Replacement Therapy (HRT) can be a powerful tool for managing symptoms like hot flashes, it is not a “weight loss pill.” Weight management is a metabolic function, not just a hormonal one. By using your blood chemistry to fix insulin sensitivity and lower systemic inflammation, you can achieve significant, sustainable weight loss regardless of whether you choose to use HRT.
Does this program work if I am already taking HRT?
Absolutely. In fact, the Advanced Metabolic Health framework often makes HRT more effective. Think of HRT as “tuning the engine” and your nutrition as the “high-quality fuel.” When your metabolism is optimized, your body can better utilize the hormones you are taking, often leading to a further reduction in symptoms like brain fog and bloating.
How long does a metabolic reset take to show results?
Most women notice a shift in their energy levels and a reduction in “puffiness” or bloating within the first 14 days of the reset. However, true metabolic repair—the kind that shifts your “Metabolic Floor”—is a 12-week process. This timeframe allows your blood chemistry to stabilize and your body to move out of chronic “survival mode.”
Is this just another “low-carb” diet?
No. Many low-carb diets actually backfire in perimenopause because they can stress the adrenals and slow the thyroid. Your Personalized Nutritional Blueprint includes the specific carbohydrates your body needs to thrive. We aren’t cutting out food groups; we are choosing the specific biological “keys” that unlock your energy.
Your Final Piece of the Puzzle: Next Steps
The weight gain, the 3 AM wake-up calls, and the soul-crushing fatigue of perimenopause are not a “new normal” you have to accept. They are signals that your internal chemistry is out of alignment.
You’ve spent years taking care of everyone else – your family, your career, your community. Now, it’s time to take a clinical, data-driven approach to your own health. Stop the guesswork, stop the “starve-and-sprint” cycle, and finally get the answers your body has been waiting for.
Are you ready to find the final piece of your metabolic puzzle?
Take Action Today:
👉 Low Friction: Download your free 24‑Hour Menopause Reset eBook and discover simple, science-backed steps to feel more balanced and energized today. Take this first step toward reclaiming your vitality
💖 High Impact: Apply for your Advanced Metabolic Health Assessment to get started with your health reset!
A Year From Now, You’ll Wish You Started TODAY!
Karen Lamb
We believe that looking after your health is essential for a fulfilling life. It enhances energy, resilience, and mental well-being, allowing you to pursue your goals. Prioritising health prevents illness, promotes longevity, and ensures you can enjoy life’s experiences to the fullest. Invest in your wellbeing and we will be there to guide you every step of the way.
We know we can help you on your wellness journey, so let’s get started!
Please call to book in a discovery call
(0431)967056

 Stop eating for someone else’s biology. 🧬 My new ebook reveals why “healthy” foods might be stalling your metabolism and how to use your blood chemistry to finally see results.
Stop eating for someone else’s biology. 🧬 My new ebook reveals why “healthy” foods might be stalling your metabolism and how to use your blood chemistry to finally see results.